|
CMS assigns hospitals two major star ratings: the HCAHPS summary star rating, based exclusively on patient survey scores; and the Overall Hospital Quality Star Rating, which incorporates outcomes measures as well as patient experience scores.
Currently, 188 hospitals have a five-star HCAHPS summary star rating and 83 have a five-star overall hospital quality star rating. The following 19 hospitals are a rare breed, as they are the only hospitals in the nation that currently have the highest possible rating — five stars — in both of those rating programs. They are listed alphabetically below.
Comments
List of alternative forms of care for the assessment panels
Community hospital or general practitioner bed Nursing home—immediate access for short term care Nursing home (elderly mentally infirm)—immediate access for short term care Respite care home—immediate access for short term care Residential home—immediate access for short term care Hospice Urgent referral for outpatient treatment or investigation—same day (including x ray) Urgent referral for outpatient treatment or investigation—next day (including x ray) Urgent home visit by consultant—within 48 hours Intensive home support—provided within 2 hours Intensive home support—provided within 12 hours Less intensive home support—provided within 12 hours Continuous minor social support in the home—provided within 2 hours Other—to be specified Consumer advocates call for hospitals to implement fair and transparent billing practices on the heels of a new Harvard report documenting medically-related bankruptcies
Boston, MA, February 2, 2005. Community Catalyst welcomes the release of “Illness And Injury As Contributors to Bankruptcy.” The report, by researchers from Harvard Law School and Harvard Medical School and published in Health Affairs, finds that almost half of all personal bankruptcies stem from medically related causes. This report confirms, in detail, what advocates have known since first monitoring hospital charity care practices. “Middle class families can see the American Dream vanish with one trip to the hospital, especially if they are uninsured or underinsured,” said Betsy Stoll, Development and Policy Director of Community Catalyst, a national health consumer advocacy group working to secure quality affordable health access for everybody. “Hospitals need to have charity care policies that help people, not force them to mortgage their homes to pay their bills. Unfortunately, this may be the tip of the bankruptcy iceberg. More and more of the cost of health care is being shifted to individuals, and at the same time we’re witnessing efforts to weaken Medicaid. This means increased pressure on hospitals and the insured and uninsured alike.” Recent lawsuits, Congressional hearings, and investigative reports have detailed many of the harsh billing and collection practices used by hospitals that leave families with no alternative but bankruptcy. In 2003, Community Catalyst released “Not There When You Need It: The Search for Free Hospital Care”, and it continues to help local consumer groups press hospitals to change their collection practices and adopt fair billing principles. “We invite hospitals to join with us in pressing for policies that protect families from financial catastrophe, and in preserving a strong health care safety net. We have a common interest in making sure that everyone has the coverage they need,” said Stoll. “There are no winners in a medical bankruptcy.” NASHVILLE — Some of the debtors sitting forlornly in this city’s old stone bankruptcy court have lost a job or gotten divorced. Others have been summoned to face their creditors because they spent mindlessly beyond their means. But all too often these days, they are there merely because they, or their children, got sick.
Wes and Katie Covington, from Smyrna, Tenn., were already in debt from a round of fertility treatments when complications with her pregnancy and surgery on his knee left them with unmanageable bills. For Christine L. Phillips of Nashville, it was a $10,000 trip to the emergency room after a car wreck, on the heels of costly operations to remove a cyst and repair a damaged nerve. American Journal of Medicine.1 Medical expenses now account for 60% of personal bankruptcy in the United States. Bankruptcies resulting from unpaid medical bills will affect nearly 2 million people this year—making health care the No. 1 cause of such filings.2
There is a heated ongoing debate about health care costs and who should decide what level of care patients should receive, doctors or insurance companies? One of the biggest challenges in health care is controlling costs. A primary way to accomplish that is keeping people out of hospitals, which are very expensive places, and paying hospitals less money. In the last year, a central front in this war on cost has been short-stay, or one-day, admissions. Insurers feel hospitals have too often been providing care that isn't necessary, and been paid too much for it.3 There are 35,416,0208 hospital admissions annually in the US. with the average length of stay at 4.8 days. Including the services provided during these stays, the cost of hospital health care annually in the United States is $859,419,233,000.4 Additionally, there are 125.7 million outpatient hospital visits annually.8 While the number of these visits that might find medically proximate lodging to be useful has not been determined, its seems likely that there is a market for these accommodations. At least in part, this business plan is an attempt to reconcile this conflict. If hospital administrators and health care professionals have an alternative to hospital admission or simple discharge that is close enough in the event of emergency to intervene and yet put the hospital at less risk of arbitrary reductions in payment for services. If Hospitalite' can provide a safe comfortable enhanced service environment for the guest, this concept will find and fill an unmet need in the marketplace. Additional research is warranted to evaluate the realistic size of the market. But if we can capture even 1 % of the 169,996,896 nights that are currently spent in hospitals, we could fill 4657 rooms at 100 % occupancy. Further, it would be valuable to engage in dialog with hospital administrators and insurance providers to ascertain the possibility of insurance companies accepting Hospitalite as a legitimate payable medical expense. Concluding with a social benefit consideration, is the potential reduction of the spiraling cost of healthcare. With the average daily cost of a hospital room in the US. at $ 1629 for a profit and $ 2025 for a non profit hospital room5, the ability to reduce a number of these stays to a cost of $ 149 +/-, could make a real difference in costs, provide a useful service and inaugurate a new profitable business model. (using the minimum figures listed above 4657room *365 *$ 1827 (avg.) = $ 3,105,543,735 annual savings) 1Medical bills prompt more than 60 percent of US. bankruptcies Article 2Medical Bills Are the Biggest Cause of US Bankruptcies: Study CNBC 3Inpatient or Outpatient? The Battle to Control Costs Source article 8 AHA 4American Hospital Association 8AHA 5Beckers Hospital Review Beckers 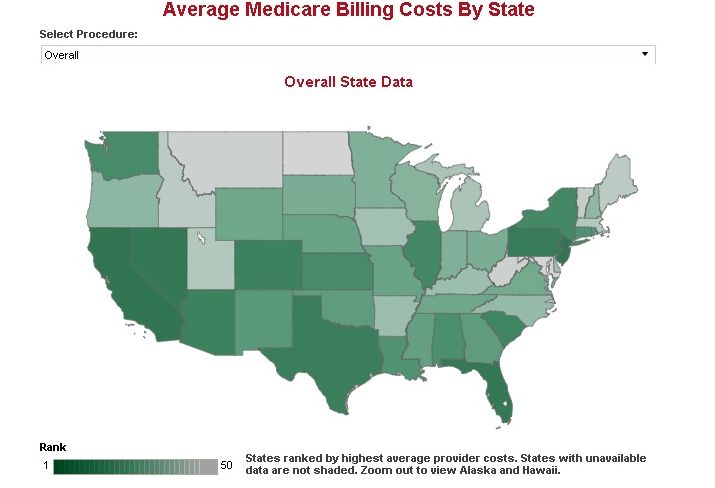 Average Hospital Cost By State Average hospital charges vary widely across the country, with many treatments costing far more in some regions than others. In addition, health costs also differ greatly among hospitals within the same region. The Centers for Medicare and Medicaid Services published data on average hospital charges for the 100 most common diagnosis and treatments for every hospital in the country treating Medicare patients. Governing compiled average hospital costs for various treatments, ranking states by cost. The following states were found to have the highest average aggregate rankings, indicating the most expensive medical costs: 1. California 2. New Jersey 3. Nevada 4. Florida 5. Pennsylvania 6. Texas 7. Alaska 8. Colorado 9. Arizona 10. South Carolina Select a procedure type in the menu below to view average provider charges and total hospital discharges by state for fiscal year 2011. Please note that listed medical charges are not the same as what patients actually pay for a service. Learn About Tableau Source: CMS Medicare Provider Analysis and Review (MEDPAR) inpatient data, FY 2011 Health Coverage
32. Roughly 10.3 million adults in America gained health coverage between January 2012 and June 2014, according to a study published in The New England Journal of Medicine. 33. The number of uninsured Americans dropped by 3.8 million from January to March, which brought the average percentage of people without health insurance to 13.1 percent, according to a survey by the Centers for Disease Control and Prevention's National Center for Health Statistics. 34. On average, healthcare cost nearly $9,000 per person in 2012, according to the Bureau of Labor Statistics. 35. On average, healthcare for a typical family of four covered by an employer-sponsored preferred provider organization plan currently costs roughly $23,215. That cost is nearly twice what it was a decade ago but the year-over-year increase of 5.4 percent between 2013 and 2014 is the lowest growth rate recorded by the Milliman Medical Index since it was first calculated in 2002. 36. National healthcare spending is projected by CMS to increase 4.7 percent from 2013 to 2015. Total Number of All U.S. Registered * Hospitals 5,627
Number of U.S. Community ** Hospitals 4,926 Number of Nongovernment Not-for-Profit Community Hospitals 2,870 Number of Investor-Owned (For-Profit) Community Hospitals 1,053 Number of State and Local Government Community Hospitals 1,003 Number of Federal Government Hospitals 213 Number of Nonfederal Psychiatric Hospitals 403 Number of Nonfederal Long Term Care Hospitals 75 Number of Hospital Units of Institutions (Prison Hospitals, College Infirmaries, Etc.) 10 Total Staffed Beds in All U.S. Registered * Hospitals 902,202 Staffed Beds in Community** Hospitals 786,874 Total Admissions in All U.S. Registered * Hospitals 34,878,887 Admissions in Community** Hospitals 33,066,720 Total Expenses for All U.S. Registered * Hospitals $892,701,370,000 Expenses for Community** Hospitals $808,869,209,000 Number of Rural Community** Hospitals 1,855 Number of Urban Community** Hospitals 3,071 Number of Community Hospitals in a System *** 3,183 Number of Community Hospitals in a Network **** 1,619 |
AuthorRobert Brooks Builder Developer Entrepreneur Seeker Archives
May 2018
Categories |

 RSS Feed
RSS Feed
